Thrombolysis lead to better long-term outcome in Chinese stroke patients
Abstract
Aim: The rate of thrombolysis in Chinese acute ischemic stroke (AIS) was low and little was known about the long-term outcome. We aimed to compare the prognosis between thrombolysis and ordinary anti-platelet strategies in AIS.
Methods: Patients, who were consecutively registered in our hospital from January 2005 to June 2012, were retrospectively studied. Inclusion criteria: (1) primary diagnoses of cerebral infarction coded with implantable cardioverter defibrillator-10 I63 to I69; (2) symptoms onset to treatment time (OTT) within 6 h; (3) thrombolysis with alteplase (TROM) or ordinary anti-platelet therapy (ANTP). Exclusion criteria: (1) symptoms and signs diminished rapidly without apparent neurological deficits; (2) no visible lesions on diffusion weighted image in magnetic resonance imaging; (3) cerebral infarction caused by serious metabolic in-balance or infections. The endpoints were defined as favorable (modified Rankin Scale 0-2) or being survival. Proportions of favorable outcome or survival were estimated by Kaplan-Meier curve and Cox regression.
Results: One hundred and sixty eight cases were analyzed. Ninety one were in TROM and 77 in ANTP. Male accounted for 82 (48.8%) and female 86 (51.2%). The median of age was 74 [interquartile range (IQR) 67-79], national institute of health stroke scale (NIHSS 9) (IQR 5-17) and OTT 3.9 h (IQR 3.0-4.8) respectively. The median length of follow-up was 112 (IQR 63.4-163.8) weeks. By the end of December 31, 2012, 87 patients (51.8%) reached favorable outcome while 81 (48.2%) unfavorable. Forty five (26.8%) cases deceased. Kaplan-Meier curve estimation showed a longer favorable period of time in TROM than those in ANTP (212 weeks 95% confidence interval (CI) 169.5-254.5 vs. 126.9 weeks 95% CI 105.2-148.6; Log-Rank test x2 = 19.632, P = 0.000), while no significance was seen in survival time (258.0 weeks 95% CI 231.5-284.5 vs. 160.8 weeks 95% CI 153.0-168.5; Log-Rank test x2 = 2.427, P = 0.119). In Cox regression, thrombolysis showed an independent protective effect for longer period of favorable outcome [202 vs. 151 weeks, P = 0.026, heart rate (HR) 1.96, 95% CI 1.958-3.540] and longer survival time instead (333 vs. 170 weeks, P = 0.000, HR 4.322, 95% CI 1.942-9.618). The estimated proportion of favorable outcome in Chinese urban AIS was about 91% for 1 year and 50% for about 3.4 years, while the estimated proportion of survival was about 98.5% for 1 year and 50% for about 5.3 years, respectively.
Conclusion: Chinese urban AIS patients who underwent thrombolysis with alteplase might have a better long-term outcome than those receiving ordinary anti-platelet therapy.
Keywords
Introduction
Thrombolysis with alteplase had been proven to be most effective in acute ischemic stroke (AIS) and its long-term good effects were verified by the Third International Stroke Trial 3.[1] In China the rate of thrombolysis of AIS was low, perhaps due to the fear of bleeding or conceptions of no need to treat mild stroke.[2] There is still no controlled study concerning the long-term outcome in Chinese AIS. Even in patients with lacunar infarction, which account for nearly 37% of total AIS and supposed to be "mild", did not reach a favorable end.[3] We aimed to compare the prognosis between thrombolysis and ordinary anti-platelet strategies in Chinese AIS.
Methods
Our hospital is one of the tertiary teaching institute attached to the Guangzhou Medical University, which is financed by government and located in the central downtown of Guangzhou city, having a total of 1,200 beds and supplies emergency medical services covering 1.5 million residents and admits more than 500 documented stroke patients each year. The number of inhabitants in the city has exceeded 12 million. One of the authors (LN) was ever a collaborator of the Imaging-based Thrombolysis Trial in Acute Ischemic Stroke-II.[4]
We searched the patients who had been consecutively registered in our database from January 2005 to June 2012. The survey was approved by The Ethics Committee of the First Affiliated Hospital of Guangzhou Medical University. The inclusion criteria were the following: (1) primary diagnoses of cerebral infarction coded with International Classification of Diseases 10th edition I63 to I69; (2) symptoms onset to treatment time within 6 h; (3) thrombolysis with alteplase as per NINDS Trial protocol or ordinary anti-platelet therapy such as aspirin and clopidegrel. Exclusion criteria included: (1) symptoms and signs diminished rapidly without apparent neurological deficits; (2) no visible lesions on diffusion weighted image in magnetic resonance imaging; (3) cerebral infarction caused by serious metabolic in-balance or infections. Patients were divided into thrombolysis group and ordinary anti-platelet one. The endpoints were defined as favorable (modified Rankin Scale 0-2) or survival. Follow-up were conducted through December, 2012 by structured telephone interview.
Data for variables nearest to the time point of treatment were collected using Microsoft® Office Excel 2003 (Microsoft Corporation, Redmond, WA, USA). The variables included demographics, vital signs, laboratory tests and radiological manifestations. Known risk factors such as cardiac abnormalities, hypertension and diabetes, smoking and prior stroke were included. The time elapse before treatment was recorded. National institute of Health Stroke Scale (NIHSS) scores were recorded in documents and reviewed by an author (WY) who had passed the NIHSS training course in 2009.
Statistical analysis
For baseline independent variables, quantitative missing values were replaced by linear regression estimates. We used binary correlations to test the collinearities of independent variables and made combinations or reductions under professional considerations. Differences between groups were tested by Mann-Whitney U-test, Pearson Chi-square and Fisher’s exact test. In Kaplan-Meier curve estimation and Cox regression, log rank test and backward step-wise likelihood chi-square test were used respectively. The inclusion and exclusion criterion of stepping probability was 0.05 and 0.10 respectively. α = 0.05 (two sided) was considered significant. Data were calculated by IBM® SPSS® Statistics version 19.
Results
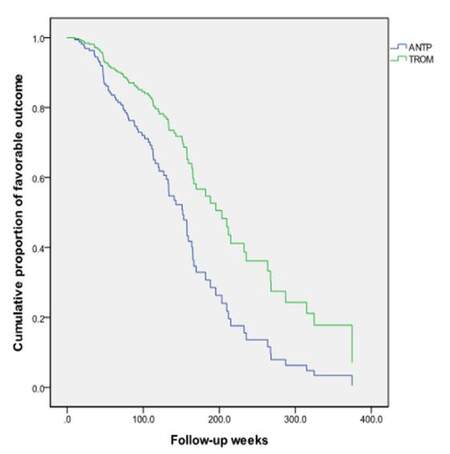
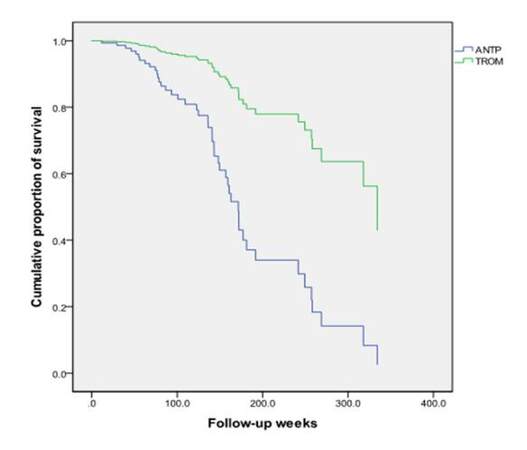
Of the 2,949 AIS patients screened, one hundred and eighty three met the inclusion and exclusion criteria. Fifteen patients lost follow-up. One hundred and sixty eight individuals entered the final analyses. Ninety one were included in thrombolysis group (TROM) and 77 in anti-platelet (ANTP) one. Male accounted for 82 (48.8%) and female 86 (51.2%). The median of age was 74 [interquartile range (IQR) 67-79], NIHSS 9 (IQR 5-17) and onset to treatment time 3.9 h (IQR 3.0-4.8) respectively. The median length of follow-up was 112 (IQR 63.4-163.8) weeks. Differences of variables between two groups were listed in Table 1. Patients in TROM were younger, had higher NIHSS scales and lower serum troponin level, higher proportion of total anterior cerebral infarction, more hemorrhagic transformations and higher proportions of hypertension, heart abnormalities and family history of stroke. By the end of December 31, 2012, eighty seven patients (51.8%) reached favorable outcome while 81 (48.2%) unfavorable. Death occurred in 45 (26.8%) cases. No significant differences were detected between TROM and ANTP. In Kaplan-Meier curve estimation, patients in TROM showed a longer favorable period of time than those in ANTP [212 weeks 95% CI 169.5-254.5 vs. 126.9 weeks 95% confidence interval (CI) 105.2-148.6; Log-Rank test x2 = 19.632, P = 0.000], while no significance was seen in survival time (258.0 weeks 95% CI 231.5-284.5 vs. 160.8 weeks 95% CI 153.0-168.5; Log-Rank test x2 = 2.427, P = 0.119). After adjusting covariates of age, gender and NIHSS, international normalized ratio, high sensitivity C reactive protein, heart failure, diabetes and interaction of NIHSS and thrombolysis in Cox regression, thrombolysis in AIS showed an independent protective effect for longer period of favorable outcome [202 vs. 151 weeks, P = 0.026, heart rate (HR) 1.96, 95% CI 1.958-3.540]. While adjusted for factors of white blood cell count, onset to treatment time and serum bicarbonate level, serum creatinine level and interaction of NIHSS and white blood cell count additionally, thrombolysis itself might be an independent predictor for longer survival instead (333 vs. 170 weeks, P = 0.000, HR 4.322, 95% CI 1.942-9.618) [Figures 1 and 2]. The estimated proportion of favorable outcome was about 91% for 1 year and 50% for about 3.4 years (4.2 vs. 3.1), while the estimated proportion of survival was about 98.5% for 1 year and 50% for about 5.3 years (6.9 vs. 3.5).
Main differences of variables between thrombolysis and anti-platelet groups
| Variables | TROM (n = 91) | ANTP (n = 77) | Z/χ2 | P value |
|---|---|---|---|---|
| Demographics | ||||
| Gender (male), n (%) | 39 (23.2) | 43 (25.6) | 2.815 | 0.121 |
| Age (years), median (IQR)* | 72 (14) | 76 (12) | -2.779 | 0.005 |
| Length (w), median (IQR)* | 149.6 (140.9) | 90.7 (69.6) | -3.463 | 0.001 |
| OTT (h), median (IQR) | 3.7 (1.5) | 4.2 (2.2) | -1.855 | 0.064 |
| Vital signs | ||||
| NIHSS Scale, median (IQR)* | 13 (11) | 5 (5) | -7.443 | 0.000 |
| BT (°C), median (IQR) | 36.5 (0.6) | 36.5 (0.5) | -0.140 | 0.889 |
| HR (/min), median (IQR) | 80 (19) | 80 (18) | -0.151 | 0.880 |
| BPS (mmHg), median (IQR) | 154 (35) | 150 (41) | -0.997 | 0.319 |
| BPD (mmHg), median (IQR) | 85 (21) | 80 (21) | -1.951 | 0.051 |
| Laboratory tests | ||||
| WBC (×109/L), median (IQR) | 8.66 (3.98) | 8.77 (2.27) | -0.347 | 0.729 |
| PLT (×109/L), median (IQR) | 218.00 (68.00) | 206.70 (65.00) | -0.275 | 0.783 |
| HCT, median (IQR) | 0.39 (0.05) | 0.38 (0.08) | -1.653 | 0.098 |
| INR, median (IQR) | 1.02 (0.21) | 1.06 (0.11) | -1.132 | 0.258 |
| APTT (s), median (IQR) | 34.40 (5.60) | 34.90 (4.53) | -0.939 | 0.348 |
| FIB (g/L), median (IQR) | 3.45 (1.09) | 3.45 (0.92) | -1.187 | 0.235 |
| Hs-CRP (mg/L), median (IQR) | 11.33 (17.99) | 10.37 (20.01) | -0.672 | 0.502 |
| GLU (mmol/L), median (IQR) | 7.70 (3.40) | 7.84 (1.84) | -0.624 | 0.533 |
| Bicarbonate (mmol/L), median (IQR) | 23.50 (3.50) | 23.17 (2.40) | -0.178 | 0.858 |
| TG (mmol/L), median (IQR) | 1.05 (0.67) | 1.04 (0.71) | -0.516 | 0.606 |
| CH (mmol/L), median (IQR) | 5.04 (1.57) | 4.95 (1.11) | -0.196 | 0.845 |
| TPR (mg/L), median (IQR)* | 0.04 (0.17) | 0.14 (0.30) | -2.237 | 0.025 |
| TP (g/L), median (IQR) | 64.20 (8.50) | 62.73 (5.50) | -1.565 | 0.118 |
| ALT (iu/L), median (IQR) | 19.00 (10.00) | 19.48 (9.39) | -0.105 | 0.916 |
| CR (mmol/L), median (IQR) | 80.00 (33.50) | 87.00 (33.35) | -1.004 | 0.315 |
| TOAST classifications | ||||
| Atherosclerotic, n (%) | 63 (37.5) | 56 (33.3) | ||
| Cardiac embolism, n (%) | 22 (13.1) | 17 (10.1) | 0.288 | 0.866 |
| Small artery, n (%) | 6 (3.6) | 4 (2.4) | ||
| OCSP classifications* | ||||
| Total anterior, n (%) | 18 (10.7) | 4 (2.4) | ||
| Partial anterior, n (%) | 49 (29.2) | 48 (28.6) | ||
| Posterior, n (%) | 16 (9.5) | 18 (10.7) | 7.993 | 0.046 |
| Lacunar, n (%) | 8 (4.8) | 7 (4.2) | ||
| Hemorrhagic transformations* | ||||
| None, n (%) | 70 (41.7) | 74 (44.0) | ||
| Hemorrhagic Infarction, n (%) | 9 (5.4) | 3 (1.8) | 14.042 | 0.001 |
| Parenchymal, n (%) | 12 (7.1) | 0 (0) | ||
| Risk factors | ||||
| Hypertension, n (%)* | 64 (38.1) | 42 (25.0) | 4.463 | 0.038 |
| Diabetes, n (%) | 23 (13.7) | 17 (10.1) | 0.235 | 0.717 |
| Heart arrhythmia, n (%)* | 20 (11.9) | 6 (3.6) | 6.416 | 0.017 |
| Heart failure, n (%)* | 29 (17.3) | 9 (5.4) | 9.704 | 0.003 |
| Smoking, n (%) | 24 (14.3) | 26 (15.5) | 1.090 | 0.314 |
| Stroke history, n (%) | 19 (11.3) | 13 (7.7) | 0.432 | 0.559 |
| Family history of stroke, n (%)* | 7 (4.2) | 0 (0) | 6.181 | 0.016 |
| Outcome | ||||
| Favorable, n (%) | 44 (26.2) | 43 (25.6) | 0.938 | 0.356 |
| Deceased, n (%) | 30 (17.9) | 15 (8.9) | 3.868 | 0.056 |
Figure 1. Cox regression. Estimation of favorable outcome proportions between TROM and ANTP. TROM: thrombolysis group; ANTP: anti-platelet group; P = 0.026
Discussion
In this hospital-based retrospective cohort study, we found thrombolysis with alteplase might have a protective effect for longer period of time of favorable outcome and survival in Chinese AIS patients. To our knowledge, this is the first observational survey that compared the long-term prognoses of thrombolysis and anti-platelet therapy in mainland China. The overall estimated five-year survival rate was 50%, comparable to published data.[5] Wang et al.[6] found one-year survival rate of hospitalized AIS patients was about 89.2% in west China, much lower than that one in our cohort (98.5%). This may due to the fact that they enrolled patients with symptoms onset within 14 days. Much of them might not have received timely thrombolytic or anti-platelet therapies. With time elapsed, stroke might progress and leading to a worse end. Notably, much of patients in their data set were mild stroke (median NIHSS score 5) with high proportion of small artery occlusion (42.9%), while we enrolled more severe patients (median NIHSS score 9) with 70.8% large artery occlusion sub-type. These results might remind the importance of timely and fully managements of mild stroke, which is more common in Chinese population with unfavorable outcome,[3,7] to reach a longer survival.
Compared to that of Gensicke et al.[8] in Switzerland, Chinese AIS patients received thrombolytic therapy seemed to have longer 50% survival time (6.9 vs. 4.0 years) and good outcome (4.2 vs. 3.0 years). We cannot make a conclusion due to the disparities of pre-defined endpoint (mRs 0-1 in Swiss vs. 0-2 in CHN) but the stroke severity was comparable (NIHSS 13 vs.14), which had been proven to be the most important determinant of stroke mortality.[9] Although Asian ethnic patients in US had higher mortality rate in hospital stay after thrombolysis,[10] and we too previously reported a higher 3-month mortality rate of 18%[11] than that in western countries,[12] further study should be performed to clarity the potential benefits of thrombolysis for long-term survival in Chinese patients, with prospective design and less bias.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
1. Group TIC. Effect of thrombolysis with alteplase within 6 h of acute ischaemic stroke on long-term outcomes (the third International Stroke Trial [IST-3]): 18-month follow-up of a randomised controlled trial. Lancet Neurol 2013;12:768-76.
2. Wang Y, Liao X, Zhao X, Wang DZ, Wang C, Nguyen-Huynh MN, Zhou Y, Liu L, Wang X, Liu G, Li H, Wang Y; China National Stroke Registry Investigators. Using recombinant tissue plasminogen activator to treat acute ischemic stroke in China: analysis of the results from the Chinese National Stroke Registry (CNSR). Stroke 2011;42:1658-64.
3. Fang XH, Wang WH, Zhang XQ, Liu HJ, Zhang HM, Qin XM, Wang ZC, Ji XM, Li LM. Incidence and survival of symptomatic lacunar infarction in a Beijing population: a 6-year prospective study. Eur J Neurol 2012;19:1114-20.
4. Wang Y, Liao X, Zhao X, Wang C, Liu L, Zhou Y, Wang C, Xue J, Gao P, Dong K, Ji X, Wang Y; ITAIS-II investigators. Imaging-based thrombolysis trial in acute ischemic stroke-II (ITAIS-II). Int J Stroke 2009;4:49-53.
5. Askoxylakis V, Thieke C, Pleger ST, Most P, Tanner J, Lindel K, Katus HA, Debus J, Bischof M. Long-term survival of cancer patients compared to heart failure and stroke: a systematic review. Bmc Cancer 2010;10:105.
6. Wang D, Hao Z, Tao W, Kong F, Zhang S, Wu B, Lin S, Liu M. Acute ischemic stroke in the very elderly Chinese: risk factors, hospital management and one-year outcome. Clin Neurol Neurosurg 2011;113:442-6.
7. Wang L, Chao Y, Zhao X, Liu L, Wang C, Wang DZ, Meng X, Wang A, Wang Y, Xu Y. Factors associated with delayed presentation in patients with TIA and minor stroke in China: analysis of data from the China National Stroke Registry (CNSR). Neurol Res 2013;35:517-21.
8. Gensicke H, Seiffge DJ, Polasek AE, Peters N, Bonati LH, Lyrer PA, Engelter ST. Long-term outcome in stroke patients treated with IV thrombolysis. Neurology 2013;80:919-25.
9. Schwamm LH, Fonarow GC, Reeves MJ, Pan W, Frankel MR, Smith EE, Ellrodt G, Cannon CP, Liang L, Peterson E, Labresh KA. Get With the Guidelines-Stroke is associated with sustained improvement in care for patients hospitalized with acute stroke or transient ischemic attack. Circulation 2009;119:107-15.
10. Nasr DM, Brinjikji W, Cloft HJ, Rabinstein AA. Racial and ethnic disparities in the use of intravenous recombinant tissue plasminogen activator and outcomes for acute ischemic stroke. J Stroke Cerebrovasc Dis 2013;22:154-60.
11. Niantong L, Ling C, Biping Y. Predictors of mortality in acute ischemic stroke patients with thrombolysis. Shi Yong Yi Xue Za Zhi 2013:2861-3.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Lin NT, Cao YC, Cheng ZZ, Wang Y, Xu PY. Thrombolysis lead to better long-term outcome in Chinese stroke patients. Neurosciences 2016;3:98-101. http://dx.doi.org/10.20517/2347-8659.2015.46
AMA Style
Lin NT, Cao YC, Cheng ZZ, Wang Y, Xu PY. Thrombolysis lead to better long-term outcome in Chinese stroke patients. Neuroimmunology and Neuroinflammation. 2016; 3: 98-101. http://dx.doi.org/10.20517/2347-8659.2015.46
Chicago/Turabian Style
Lin, Nian-Tong, Ying-Chun Cao, Zheng-Zheng Cheng, Yuan Wang, Ping-Yi Xu. 2016. "Thrombolysis lead to better long-term outcome in Chinese stroke patients" Neuroimmunology and Neuroinflammation. 3: 98-101. http://dx.doi.org/10.20517/2347-8659.2015.46
ACS Style
Lin, N.T.; Cao Y.C.; Cheng Z.Z.; Wang Y.; Xu P.Y. Thrombolysis lead to better long-term outcome in Chinese stroke patients. Neurosciences. 2016, 3, 98-101. http://dx.doi.org/10.20517/2347-8659.2015.46
About This Article
Copyright
Author Biographies

Data & Comments
Data
 Cite This Article 0 clicks
Cite This Article 0 clicks











Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.